
After a stroke, eating well is more than just fuelling the body, it supports cognitive function, muscle strength, and immune health, while helping to prevent complications such as malnutrition and dehydration. However, many stroke survivors face difficulties with eating due to challenges such as dysphagia (difficulty swallowing) or reduced appetite.
Did you know?
Dysphagia can affect up to half of stroke survivors. It not only increases the risk of choking, but can also cause aspiration pneumonia, a lung infection that occurs when food or liquid accidentally enters the airway. Dehydration and poor nutrition are also common, which can slow down recovery. Some may also experience loss of appetite, fatigue, or difficulty recognizing hunger, further worsening their nutritional status.
To make eating safer, foods and liquids are often texture-modified. This helps stroke survivors swallow more easily without choking. The International Dysphagia Diet Standardisation Initiative (IDDSI) provides a global framework with eight levels (0–2 for liquids and 3–7 for foods) that define the right texture and thickness for everyone. Speech therapists assess each patient and determine the appropriate IDDSI level. These guidelines help caregivers prepare meals that are both safe and satisfying.
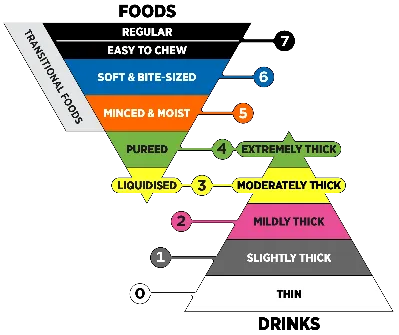
Despite its benefit, a texture-modified diet can be challenging. Meals may appear bland or watery, and thickened fluids can make hydration difficult. Many lose interest in eating due to unappealing textures or repetitive flavours, increasing the risk of malnutrition.

Choose wisely: Incorporate nourishing options like Greek yogurt, pureed lentils, soft tofu, mashed sweet potatoes, or smooth nut butters. These foods pack in energy even in small portions.

Enrich it: Boost nutrition by adding powdered milk, cheese, full-fat yogurt, or eggs to porridge, soups, or mashed dishes. Use milk or broth instead of water to blend foods for better nutrition and taste.

Small but frequent: Instead of three large meals, aim for smaller, more frequent meals to maintain energy and prevent fatigue during eating. When appetite is poor, oral nutritional supplements can help meet daily needs.

Make it look good: Use food moulds or plating techniques to make pureed foods look like their original shape. This enhances appetite and restores mealtime dignity.

Hydrate smartly: Stay hydrated with naturally thicker liquids like milkshakes and fruit smoothies, or yogurt drinks. Encourage small, frequent sips throughout the day.

Keep to regular meal and snack times: Routine promotes consistency and ensures adequate intake.

Serve familiar favourites: Where possible, adapt favourite foods from before the stroke to the appropriate texture level, familiar flavours spark comfort and stimulate appetite.

Create a calm eating space: A quiet, relaxed environment allows better focus on swallowing safely and makes meals more enjoyable.
If you or your loved one is struggling with poor appetite, weight loss, or difficulty adjusting to texture-modified foods, consult a dietitian. A dietitian can help:
With the right guidance and a little creativity, every meal can once again bring comfort, strength, and healing.

Good nutrition does not end with recovery; it plays a crucial role in preventing another stroke. Once swallowing improves, focus on a heart-healthy diet rich in fruits, vegetables, whole grains, lean protein, and healthy fats. Reducing salt, sugars, and unhealthy fats helps control blood pressure, and maintain healthy cholesterol levels, all of which lower the risk of another stroke.
Written by Dietitians of Pantai Hospital Penang

