Artikel pendidikan ini ditulis oleh Dr. Sze Xun Quan, Pakar Perunding Nefrologi, untuk membantu anda memahami kesihatan buah pinggang dengan lebih baik.
Buah pinggang ialah organ penting yang berfungsi untuk:
- Menyingkirkan sisa nitrogen (toksin)
- Mengawal keseimbangan air dalam badan (melalui pengeluaran air kencing)
- Mengawal elektrolit dalam badan (Natrium, Kalium)
- Mengekalkan keseimbangan asid-bes dalam badan
- Mengawal paras hemoglobin dengan menghasilkan hormon eritropoietin
Walau bagaimanapun, penyakit buah pinggang adalah lazim dan sering menjadi komplikasi kepada penyakit kronik (seperti Diabetes Mellitus dan Hipertensi). Penyakit Buah Pinggang Kronik (CKD) juga kerap berlaku, melibatkan kira-kira 10–15% populasi di seluruh dunia.
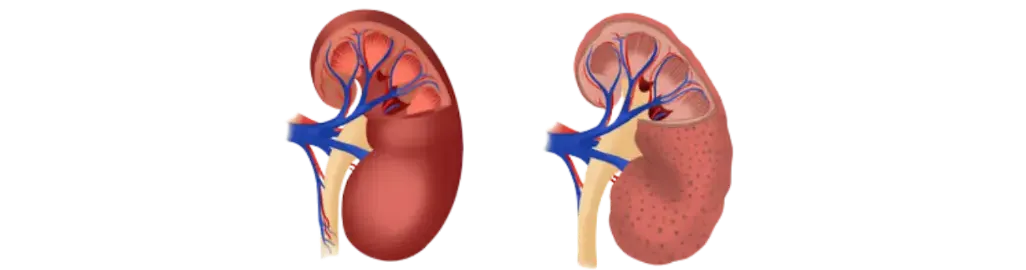
Normal CKD
Apakah itu penyakit buah pinggang kronik (CKD)?
Jawapan: CKD ialah keadaan di mana paras kreatinin tidak normal dan/atau terdapat albumin atau darah dalam air kencing secara berterusan selama lebih 3 bulan.
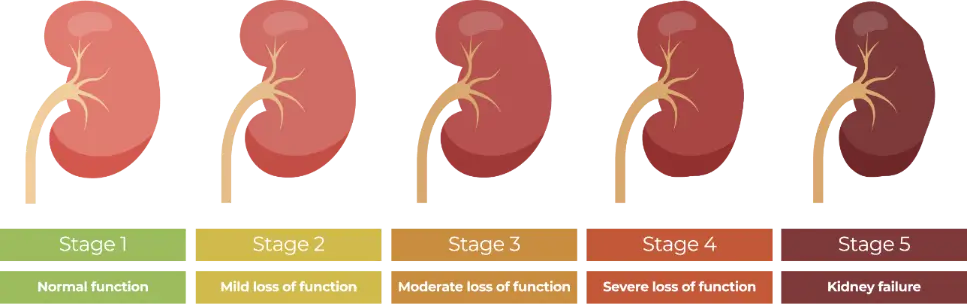
Berapa tahap CKD yang ada?
Jawapan: 5 tahap
- Tahap 1: GFR > 90
- Tahap 2: GFR 60–89
- Tahap 3: GFR 30–59
- Tahap 4: GFR 15–29
- Tahap 5: GFR < 15
Apakah punca CKD?
Jawapan:
- Diabetes
- Hipertensi
- Penyakit glomerular
- Penyakit buah pinggang polikistik
- Ubat-ubatan (terutamanya penggunaan NSAID yang kerap)
- Batu karang yang menyebabkan penyumbatan saluran kencing atau jangkitan
Bolehkah ia disembuhkan?
Jawapan:
Buat masa ini, tiada ubat yang boleh menyembuhkan CKD. Rawatan bertujuan untuk memperlahankan perkembangan kerosakan buah pinggang.
Bagaimana proses rawatan dijalankan?
- Pengambilan sejarah perubatan pesakit secara terperinci, termasuk ubat-ubatan semasa, untuk mengenal pasti punca yang mungkin menjejaskan fungsi buah pinggang (serta menolak kemungkinan kecederaan buah pinggang akut).
- Imbasan ultrabunyi buah pinggang dilakukan untuk menolak kemungkinan masalah kongenital atau penyumbatan akibat batu karang.
Pilihan rawatan bukan farmakologi:

1. Pengurangan berat badan
Berat badan berlebihan (BMI > 25) semakin lazim. Di Malaysia, 54.4% mempunyai BMI > 25 dan 21.8% adalah obes (BMI > 30). Obesiti bukan sahaja memburukkan CKD, malah meningkatkan risiko penyakit lain.

2. Senaman secara berkala
Lakukan aktiviti fizikal sederhana (5 kali seminggu, 30 minit setiap sesi). Aktiviti fizikal boleh dikategorikan kepada tahap sedentari, ringan, sederhana dan intensif.

3. Berhenti merokok
CRokok mengandungi pelbagai bahan kimia berbahaya. Nikotin dan kadmium khususnya boleh merosakkan buah pinggang.

4. Cadangan pemakanan:
- Kurangkan pengambilan garam (natrium). (Termasuk garam biasa, kicap, makanan dalam tin dan sebagainya.) Pengambilan natrium berlebihan boleh menyebabkan tekanan darah tinggi dan penyakit kardiovaskular.
Bagi pesakit CKD, pengambilan garam disarankan kurang daripada 5g sehari. - Lebihkan pengambilan buah-buahan dan sayur-sayuran.
- Kurangkan makanan tinggi protein (sebaiknya rujuk doktor, kerana pengambilan protein yang terlalu rendah juga boleh menyebabkan malnutrisi).

5. Elakkan penggunaan ubat atau suplemen yang tidak perlu
Pengurusan Berasaskan Ubat
Seperti yang dinyatakan sebelum ini, setakat ini tiada ubat yang boleh menyembuhkan penyakit buah pinggang kronik (CKD). Rawatan yang ada bertujuan untuk memperlahankan kemerosotan fungsi buah pinggang.
1. Kawalan Gula Dalam Darah (Bagi Pesakit Diabetes)
Sasaran HbA1c: antara 6.5–8.0.
Bagi pesakit yang lebih muda atau belum mengalami komplikasi diabetes, kawalan gula dalam darah biasanya lebih ketat.
2. Sasaran tekanan darah sistolik (SBP): di bawah 120 mmHg,
namun ini bergantung pada keadaan individu. Sebagai contoh, bagi pesakit warga emas yang mungkin mengalami gejala tekanan darah rendah, berjalan tidak stabil atau berisiko tinggi untuk jatuh, sasaran tidak seharusnya terlalu rendah.
3. 4 Komponen Utama Rawatan Penyakit Buah Pinggang Diabetes
- Perencat ACE / ARB
Ini ialah sejenis ubat tekanan darah.
Selain mengawal tekanan darah dengan berkesan, ia juga membantu memperlahankan perkembangan CKD dan mengurangkan kehilangan protein (albumin) dalam air kencing.
Perencat ACE biasanya berakhir dengan “-pril”, manakala ARB biasanya berakhir dengan “-sartan”. - Perencat SGLT2
Ini ialah ubat antidiabetik, yang digunakan terutamanya untuk mengurangkan kehilangan albumin dalam air kencing.
Ia juga mempunyai kesan tambahan seperti membantu menurunkan tekanan darah dan berat badan.
Ubat ini biasanya berakhir dengan “-gliflozin”. - Penyekat MRA Bukan Steroid
Ubat ini bukan sahaja membantu mengurangkan kehilangan albumin dalam air kencing, malah turut membantu mengurangkan keradangan dan sklerosis (parut) pada buah pinggang.
Ubat ini biasanya berakhir dengan “-renone”. - Agonis GLP-1
Ini juga merupakan ubat antidiabetik yang berkesan dalam membantu menurunkan berat badan serta memperlahankan perkembangan penyakit buah pinggang.
Ubat ini biasanya berakhir dengan “-glutide”.
Keempat-empat kumpulan ubat di atas bukan sahaja membantu mengurangkan kehilangan albumin dalam air kencing dan memperlahankan perkembangan CKD, malah turut memberikan perlindungan kardiovaskular.
Walau bagaimanapun, setiap ubat mempunyai kesan sampingan tersendiri, jadi adalah penting untuk berbincang dengan doktor anda sebelum memulakan rawatan.
Artikel pendidikan ini ditulis oleh Dr. Sze Xun Quan, Pakar Perunding Nefrologi, untuk membantu anda memahami kesihatan buah pinggang dengan lebih baik. Buat janji temu anda sekarang di Hospital Pantai Batu Pahat. Anda juga boleh membuat janji temu melalui laman web kami atau dengan memuat turun apl My Health 360 di Google Play Store atau Apple App Store.











