This educational piece is written by Dr. Sze Xun Quan, Consultant Nephrologist, to help you better understand your kidney health.
What Do Kidneys Do?
The kidneys are vital organs that perform several important functions in the body, including:
- Removing waste products and toxins from the blood
- Regulating water balance by producing urine
- Maintaining electrolyte balance (such as sodium and potassium)
- Regulating acid-base balance
- Supporting red blood cell production by producing the hormone erythropoietin
Kidney disease is common and often develops as a complication of chronic conditions such as diabetes mellitus and hypertension. Globally, chronic kidney disease (CKD) affects approximately 10–15% of the population.
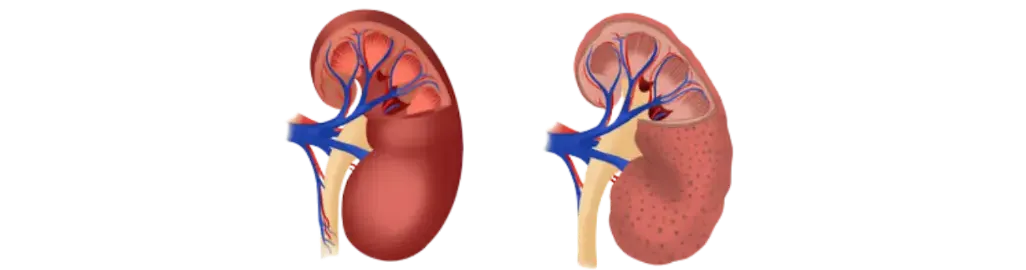
Normal CKD
What Is Chronic Kidney Disease (CKD)?
Chronic kidney disease (CKD) is a condition in which kidney function gradually declines over time. It is defined as having abnormal creatinine levels and/or persistent albumin or blood in the urine for more than 3 months.
What Are the Stages of CKD?
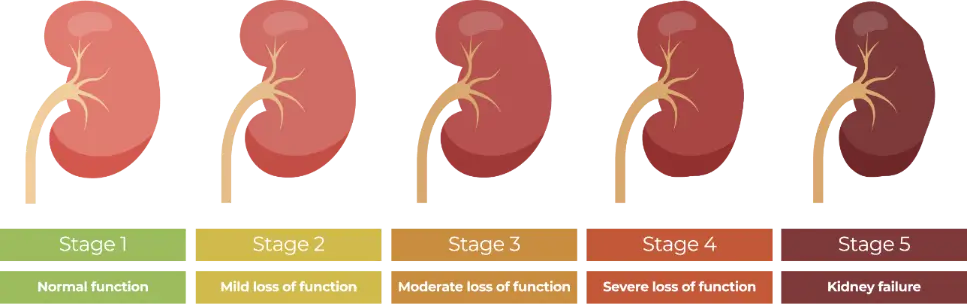
CKD is classified into five stages based on the glomerular filtration rate (GFR):
- Stage 1: GFR > 90
- Stage 2: GFR 60–89
- Stage 3: GFR 30–59
- Stage 4: GFR 15–29
- Stage 5: GFR < 15
What Causes Chronic Kidney Disease?
Common causes of CKD include:
Diabetes
Hypertension (high blood pressure)
Glomerular diseases
Polycystic kidney disease
Medications (especially frequent use of NSAIDs)
Kidney stones causing urinary tract obstruction or infection
Is There a Cure for CKD?
Currently, there is no cure for chronic kidney disease. Treatment focuses on slowing disease progression and preventing complications.
What Is the Treatment Process Like?
Evaluation typically includes:
- A detailed patient medical history, including current medications, to identify any possible cause affecting kidney function (and to rule out acute kidney injury).
- Ultrasound of the kidneys, to rule out congenital issues or obstruction from kidney stones.
Lifestyle and Non-Pharmacological Management

Weight reduction
Being overweight (BMI > 25) is increasingly common. In Malaysia, 54.4% of individuals have a BMI > 25, and 21.8% are obese (BMI > 30). Obesity can worsen CKD and increase the risk of other chronic diseases.

Regular exercise
Engage in moderate physical activity (5 times a week, 30 minutes each session).
Physical activity can be categorized into sedentary, light, moderate, and vigorous.

Quit smoking
Smoking exposes the body to harmful chemicals such as nicotine and cadmium, which can damage the kidneys.

Dietary recommendations
- Reduce salt (sodium) intake, including hidden sources such as soy sauce and processed foods. Excess sodium can cause high blood pressure and cardiovascular disease.
- For CKD patients, limit salt intake to less than 5g per day.
- Eat more fruits and vegetables.
- Adjust protein intake based on medical advice, as excessive or insufficient protein can be harmful.

Avoid unnecessary medications or supplements
Medication-Based Management
While CKD cannot be cured, medications can help slow disease progression and protect kidney function.
1. Control of blood sugar (for diabetic patients)
Target HbA1c: between 6.5–8.0.
If the patient is younger or has no diabetic complications yet, blood sugar control tends to be more stringent.
2. Blood pressure control
Target systolic blood pressure (SBP): below 120 mmHg. However, this depends on the individual case. For example, in elderly patients who may experience symptoms of low blood pressure or have unstable walking and a higher risk of falling, the target should not be set too low.
3. The four pillars of diabetic kidney disease treatment
- ACE-Inhibitors / ARBs (blood pressure medications)
These medications effectively control blood pressure, slow down the progression of CKD, and reduce the loss of protein (albumin) in urine. ACE inhibitors usually end in “-pril”, and ARBs usually end in “-sartan”. - SGLT2-Inhibitors (anti-diabetic medications)
These medications are primarily used to reduce urinary albumin loss. They also have mild effects in lowering blood pressure and reducing body weight. These drugs usually end in “-gliflozin”. - Non-Steroidal MRA Blockers
These medications help reduce urinary albumin loss, kidney inflammation, and sclerosis (scarring). These drugs usually end in “-renone”.
- GLP-1 Agonists (anti-diabetic medications)
These medications are effective in reducing body weight and slowing kidney disease progression. These drugs usually end in “-glutide”.
These medications also provide cardiovascular protection. However, each has potential side effects and should be discussed with your doctor.
How to Protect Your Kidneys
You can help protect your kidney function by:
- Controlling blood sugar levels
- Managing blood pressure
- Maintaining a healthy weight
- Following a balanced diet
- Attending regular health screenings
- Avoiding smoking
Protect Your Kidneys with Early Screening
Chronic kidney disease is a serious but manageable condition. Early detection and proper management can significantly slow disease progression and reduce complications.
This educational article is written byDr. Sze Xun Quan, Consultant Nephrologist, to help you better understand your kidney health.
Book your appointment at Pantai Hospital Batu Pahat for a comprehensive kidney function screening. You may also schedule an appointment through our website or via the My Health 360 app available on Google Play Store and Apple App Store.











