
This article was contributed by Dr Albert Tan Chao Chiet, Consultant Obstetrics & Gynaecology (O&G) - Urogynaecology at Pantai Hospital Cheras. To book an appointment or learn more about Dr Albert Tan Chao Chiet and his clinic, click here
By Dr. Albert Tan Chao Chiet, Consultant Obstetrician, Gynaecologist & Urogynaecologist
Urinary incontinence — the involuntary leakage of urine — affects countless women across Malaysia, yet many continue to suffer silently. Often dismissed as a normal consequence of childbirth, ageing, or menopause, incontinence is not something women have to “tahan sahaja”. It is a medical condition with effective, proven treatments.
Women frequently describe how incontinence affects their social life, work, exercise, and confidence. Many avoid travel, restrict fluids, or live in constant fear of leakage. With proper assessment and treatment, most women can regain full control of their bladder — and their lives.
Not all urinary leakage is benign. Sometimes, incontinence may be linked to an underlying pelvic mass or even a dangerous uterine tumour compressing the bladder, especially if symptoms develop suddenly or worsen rapidly.
Women should seek prompt evaluation if they experience:
Early diagnosis ensures that treatable problems are not overlooked — and that serious conditions are detected early.
Pelvic Organ Prolapse (POP) occurs when the bladder, womb, or bowels slips down due to weakened pelvic floor muscles — often after childbirth, difficult deliveries, menopause, or chronic coughing. Many women do not realise that prolapse and urinary incontinence often occur together.
Prolapse can cause
When prolapse is present, treating incontinence alone is often ineffective. Both conditions must be assessed and managed together, using a holistic pelvic floor approach.
This is precisely why urogynaecologists — specialists trained in both gynaecology and female pelvic floor disorders — are the most appropriate experts to diagnose and treat female incontinence. Unlike urologists, whose training focuses primarily on the urinary tract, urogynaecologists are specifically trained to evaluate how the uterus, vagina, pelvic floor muscles, and bladder interact — a crucial factor when managing conditions unique to women.
Stress urinary incontinence (SUI)—urine leakage during coughing, laughing, or physical activity— is one of the most common forms of female incontinence. When pelvic floor exercises or medications do not provide sufficient relief, surgical treatment may be indicated.
I am currently the only known urogynaecologist in Malaysia who routinely performs Laparoscopic Burch Colposuspension with consistently positive clinical outcomes. This minimally invasive, mesh-free procedure uses sutures to restore the bladder’s natural support, and is backed by decades of international evidence demonstrating its safety, durability, and long-term success.
For women who prefer to avoid synthetic mesh, or those who have experienced complications from prior mesh surgery, laparoscopic Burch colposuspension provides a reliable, effective, and proven alternative.
In the past, synthetic mesh slings were widely used to treat stress incontinence because they were quick to insert and initially effective. However, over the years, many countries have reported serious complications from mesh, including:
Several nations, including the UK and New Zealand, have imposed strict regulations or temporary bans on mesh for incontinence due to these adverse outcomes.
For women who prefer to avoid mesh, or those who have had complications from previous mesh procedures, laparoscopic Burch colposuspension offers a safe and effective alternative with a long history of success — without introducing foreign material into the body.
Female incontinence impacts self-esteem, relationships, and daily activities. But with targeted assessment, conservative therapy, and advanced surgical options like laparoscopic Burch colposuspension, women can regain normal function and confidence.
If you or someone you know experiences urinary leakage, do not ignore the symptoms. Help is available, and you do not have to live with incontinence.
For further information or to arrange a consultation, you may reach out to my affiliated clinics or book an appointment at Pantai Hospital Cheras.
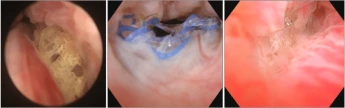
Mesh erosion in the urethra on cystourethroscopy.
Source: Han, Ji-Yeon. (2019). Recurrent Urinary Tract Infection from Urethral Mesh Erosion after
Midurethral Mesh Sling Surgery. Urogenital Tract Infection. 14. 60. 10.14777/uti.2019.14.2.60.


